Nearly 80% of people with LBD received a diagnosis for a different cognitive, movement or psychiatric disorder before ultimately learning they had Lewy body dementia (LBD), according to the Lewy Body Dementia Association’s report, Caregiver Burden in Lewy Body Dementias. 50% of the time, the original diagnosis was Alzheimer’s. LBD, the second-most common form of degenerative dementia in the elderly affecting an estimated 1.3 million people in the United States, is most often misdiagnosed as Alzheimer’s disease.
Amazon.com
Lewy Body Dementia:
What Everyone Needs to Know


A Caregiver’s Guide To
Lewy Body Dementia
Winner of The
Caregiver Friendly Award

DIAGNOSIS
Free Tool:
Looking for Lewy Body Dementia
Diagnosis Barriers
This eye-opening report reveals people with LBD and their caregivers face barriers to obtaining an early LBD diagnosis. Half of people seeking a diagnosis for LBD symptoms saw three or more doctors for 10 visits over the course of a year before they were diagnosed with LBD, and diagnosis required more than two years from the onset of symptoms for 31% of cases. Additionally, caregivers experience moderate to severe emotional burden, and most experience a sense of isolation because so few people know about LBD.
The findings are based on data collected by the Lewy Body Dementia Association (LBDA) in an online survey of 962 LBD caregivers. Designed by Steven H. Zarit, PhD, an expert on caregiver burden in dementia and Professor of Human Development at Penn State University, the survey was conducted over a 6-month period. Dr. James E. Galvin, a member of LBDA’s Scientific Advisory Council and Professor of Neurology and Psychiatry at New York University, analyzed the survey data, which was published in the July, 2010 issue of Parkinsonism & Related Disorders and the April-June, 2010 issue of Alzheimer Disease & Associated Disorders.
Symptoms of LBD
Symptoms of LBD include dementia, unpredictable variations in cognition, attention or alertness, hallucinations, Parkinson’s-like symptoms, a sleep disorder characterized by physically acting out vivid nightmares and dreams, and a potentially life-threatening sensitivity to certain medications. Changes in mood and dysfunction of the autonomic nervous system are also common in LBD. The combination of cognitive, motor and behavioral symptoms creates a highly challenging set of demands for continuing care.
LBD is an umbrella term, because LBD has several clinical presentations. Some individuals will start out with a movement disorder leading to the diagnosis of Parkinson’s disease and later develop dementia. Another group of individuals will start out with a memory disorder that may look like Alzheimer’s disease, but over time two or more distinctive features become apparent leading to the diagnosis of ‘dementia with Lewy bodies’ (DLB). Lastly, a small group will first present with neuropsychiatric symptoms, which can include hallucinations, behavioral problems, and difficulty with complex mental activities, also leading to an initial diagnosis of DLB. Regardless of the initial symptom, over time all three presentations of LBD will develop very similar cognitive, physical, sleep and behavioral features, all caused by the presence of Lewy bodies throughout the brain.
Inadequate Discussion, Lack of Info
LBD caregivers rated specialists and general practitioners as inadequate in discussing disease progression. “The lack of information on disease progression is a serious challenge to LBD families,” stated Angela Herron, President of LBDA’s board of directors. “It’s essential that families plan in advance for the relentless progression of LBD, and not having answers on what that decline will look like or how fast it may occur, adds significant stress and burden to an already difficult situation.”
Kathy Fowler struggled for 5 years to get a diagnosis for her husband Philip’s symptoms. After his quadruple by-pass in 2003, Philip’s recovery was taking a longer time than expected. Not so much physically but cognitively and emotionally. “Why was he behaving so bizarrely?” Kathy asked professional after professional. “He’s not quite right,” she would tell them. She remembers his cardiologist leaning cavalierly in the office doorway, saying , “Yeah, that happens sometimes.” Disheartened, she kept up appearances for friends and family, but privately accused her husband of drinking or taking drugs. She didn’t know that LBD, a common form of dementia she’d never heard of, was robbing him of his mind.
LBD Versus Other Dementias
Although prognosis varies among individuals, LBD is often a more rapidly progressive disease than Alzheimer’s disease, and early diagnosis provides families an opportunity to plan for expected decline in cognition, function and behavior. Unlike other dementias, people with LBD are exquisitely sensitive to certain medications, making early diagnosis a critical component to minimizing exposure to medications that may aggravate symptoms, such as antipsychotic medications. Nearly 60% of people with LBD may experience severe, potentially irreversible reactions to antipsychotic medications, and in rare cases, a life threatening condition called neuroleptic malignant syndrome may also occur. Given the evidence that suggests treatment with cholinesterase inhibitors may benefit patients with LBD more than those with Alzheimer’s disease, barriers to diagnosis have a negative impact on both the LBD patients’ and caregivers’ quality of life.
SOURCE:








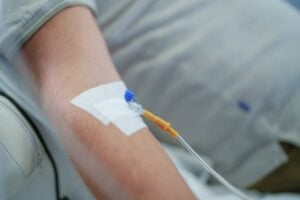


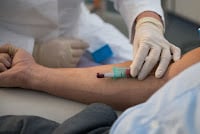


Yes it can be both !! I was the caregiver to my brother & he had both .
"people with LBD are exquisitely sensitive to certain medications, making early diagnosis a critical component to minimizing exposure to medications that may aggravate symptoms, such as antipsychotic medications" Look at the medications that the patient is taking. My mother, who is 75, was placed on an anti-depressant, high blood pressure medicine (one with diuretic, one without), cholesterol medication, potassium supplements, and a blood thinner. Living 1/2 hour away, and my father keeping her problems to himself, it just became apparent to my sisters and I within the last year of how bad she really was. Come to find out, she had been having screaming, crying fits for 3 to 4 days at a time, hallucinations, vivid dreams, confusion, severe memory loss, etc. She was a basket case, to say the least, and it was taking a terrible toll on my father. The psychologist and her regular Dr. immediately diagnosed her with Alzheimer's and early on-set dementia. I questioned the meds that she was on and checked the side effects. You have to remember that it may not be one single med, but a combination of the meds that they are taking. I had to fight tooth and nail to get the Dr. to allow me to wean her off of the anti-depressant and give me instructions on how to do so. Dr. said she could be weaned off in 2 weeks, but a lot of the time the symptoms will worsen due to the fact that she is going through withdraw and then I would have to re- up the dosage. I suggested weaning her off at a much slower pace to allow her body to adjust (3 month period). As I slowly reduced the dosage I could see changes for the better (she still had some bad days, but I refused to re-up the dosage. She stayed with me for several days of the first week, and all of the 2nd week so I could keep an eye on her reaction, and believe me, there were days when I questioned my method and was ready to re-up the dosage). At that point, I introduced raw, organic, extra virgin coconut oil (2 tsp. 3 times per day) to her diet. (For more info on coconut oil go to Dr. Newport's website) My mom has been completely off of the anti-depressant for almost 4 weeks now and is still taking the coconut oil. She has improved by 85%. She still has a few set backs, but keep in mind, it takes 4 to 6 weeks for the anti-depressant to get out of her system, even after she is no longer taking it. I am currently working on weaning her from the blood pressure medicine (with diuretic) due to the fact that the diuretic depletes potassium (she is also taking potassium supplements), if potassium is depleted it can also cause memory loss and confusion AND the cholesterol medication she is taking can also cause memory loss and confusion. At her last office visit her blood pressure was 110/64. Her cholesterol is also fine. My main question to the Dr. was " WHAT GOOD DOES IT DO TO HAVE HER ON ALL OF THESE MEDS IF SHE CAN'T ENJOY OR REMEMBER EACH DAY?" I'm still waiting on a response… The latest natural cure for Alzheimer's/Dementia is Turmeric. Go to turmericforhealth.com for information on how to make Golden Paste; although, be sure to add fresh ground pepper (this enables your body to absorb the turmeric) to your recipe for it to work. I will be trying this with my mom in the near future.
"The latest natural cure for Alzheimer's/Dementia is Turmeric. Go to turmericforhealth.com for information on how to make Golden Paste; although, be sure to add fresh ground pepper (this enables your body to absorb the turmeric) to your recipe for it to work. I will be trying this with my mom in the near future"…Your words.
There to this date 10/30/2015there is no Cure for Alzheimers or any form of dementia. I have been a part of the Alzheimer's world through taking care of my husband who had both Lewy Body and Alzheimer's and continuous research for a Alzheimers Board that I am a moderator for. Please don't give false info..don't you think if a cure had been found it would have been blasted around the world?
I wish to add I am sorry for any family that has been touched by this terrible devastating disease.
And I do pray for a cure and for all those living with this disease. I took care of my husband for 7 years. I found through trial and error the less meds the better off he was. Some meds increased his hallucinations and bad behaviors. Also dehydration and UTI can cause a LO to react as if they have some form of dementia always have this checked and the liquid consumed.
I worked with his neurologist who had an understanding of all dementia's. My husband through trial and error was only taking Aricept and 6.5MG of Seroquel at bedtime to help him sleep. I would suggest always asking for the lowest doesage of a new med..more could be added if needed but it also can be gradually stopped if you see it makes a negative change in your LO. Keep a journal of the changes and take to their doctor. What worked for us was my remaining calm no matter what is happening..walk into the next room if you have to. Reassuring my husband that I was there for him with lots of HUGS and I understand..I am here for you. Simplifying every thing..keeping sentences short and simple…redirecting his thoughts by introducing perhaps lets have ice cream..whatever a loved one might still remember that brings him or her comfort. Listen even if its the third time they have said the same thing..don't say you have already told me that. His or her thinker is sadly broken. Music is really important..TV can bring on bad behaviors through loud commercials et. Keep a journal of where a LO is and what was he or she doing when a bad behavior occured..try to avoid that same place and situation again. Remember The Alzheimer's Association in your area is your friend. They can recommend a doctor who understands dementia, et. They care about you. AD has been a part of my life for 10 years..it is hard but you can do it. Always be kind to your self knowing your doing the best that you can and no one not even your self can ask for more..and prayer is your friend : )…alice
Can it be both? A year ago diagnosis Parkinson's,with dementia typical gait, at rest tremors, hallucinations.memory loss. Now a year later of living with us, and being able to observe and have several apts with neurologist, Lewy bodies symptoms seem present, horrible hallucinations, bouts of decline, then a rally back repeat. But this last decline has been much worse and has lasted a month..vist to neurologist yesterday, wouldmseem lewy bodies is possible…in which case I sm now reading eveything abou in order to prepare our family
My husband has been to 15 doctors neurologists, oncologists, spine, orthopedic, for everything from back problems to falling and not one will accept my suggestion that he has Parkinson's or something like it. He is 83 and he shuffles with arms dangling forward, his leg and arms will jerk, he has a resting tremor in his hands. He in unstable when he walks and has fallen 4 times. He has flares of mental anguish and anger and complains of feeling like he is going to fall backwards. He has always taken care of himself but these past two years he has gone downhill. What do I do? He is getting so hard to live with. If I knew there was a medical condition I could be more sympathetic.
There are many drugs that have side effects in the elderly that can mimic Parkinsonism. If your husband is on medications you may want to look in to the medication. Here is a link that explains.
http://www.medscape.org/viewarticle/586881_2
Rosebudi: Falling backwards (retropulsion) can be a symptom in Progressive Supranuclear Palsy. Falling is also a common symptom in this disease. It's important to find a neurologist who understands this disease and can determine whether or not he has it.
My husband and I had the same journey as Kathy Fowler – just wonder how common this is after heart surgery (Ken had a quadruple by pass) never was the same after but stayed at a low cognitive impairment for years before things started to change. Also took years for diagnosis – wasn't diagnosed until it was advanced. Sometimes it is just helpful to have your beliefs validated by someone. No one in the medical profession did that for me.
But as I understand, there is no definitive test for LBD – it's purely based on observed symptoms. How do we know which it is – LBD, Alzheimer's or Parkinson's with dementia???
I hope to hear more info on this as well. From what Ii have gone through, it seems that the NeuroPsych evaluations and MRI's indicate different types of behavior and different areas of the brain that atrophy vs Alzheimer's. My spouse was diagnosed with LBD (not with Parkins's) about 18 months ago. Prior to that he had been incorrectly treated for Alzheimer's and possibly Frontal Lobe Dementia by two different practitioners. We are now seeing his 3rd Physician for Dementia treatment. He has been "Not right" for 6 1/2 – 7 years . He will be 74 in July. I definitely agree with the information regarding medications… We went through the hallucinations stage almost two years ago.
It is important to see a doctor who is informed about LBD so he or she can recognize the differences. The Lewy Body Dementia Association has an excellent website that explains the differences. My husband had a DaT scan at Mayo which facilitated the confirmation of his diagnosis of LBD. The right doctor is key.
https://www.lbda.org/is-it-lbd-or-something-else/