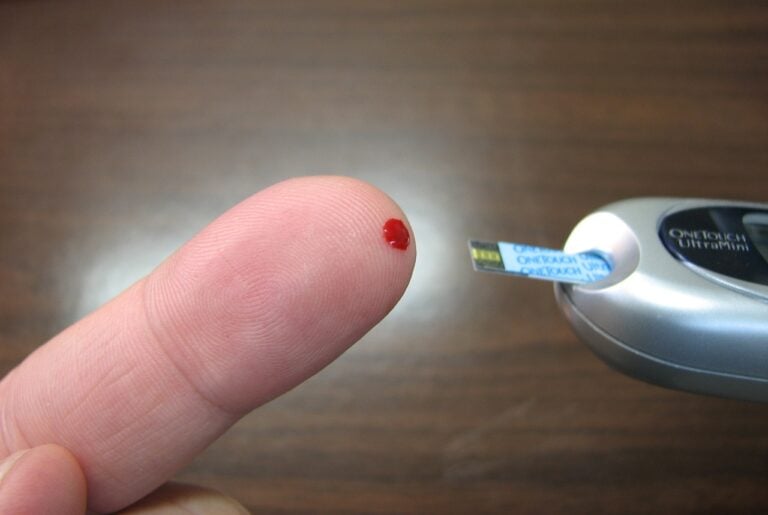
Quest Diagnostics has introduced the QUEST AD-Detect™ Amyloid Beta 42/40 Ratio, an analytically validated blood test that aids in assessing the risk of AD.
The laboratory-developed test is designed to be used by a healthcare provider to help assess the risk of AD in a patient.
Amazon Books & Videos
about Alzheimer’s and Dementia:
FREE Newsletter:
The blood test evaluates the ratio of two peptides of amyloid beta, Aβ42 and Aβ40, in plasma sourced from a single blood test and is designed to monitor Aβ42/40 changes over time to assess the risk potential of AD progression.
The test is a high-precision assay of a type shown in a recently published study to be as effective as traditional methods.
Do people want AD blood tests?
On behalf of Quest Diagnostics, The Harris Poll conducted two online surveys in March 2022: one among 501 US duly licensed primary care providers (PCPs) with a patient load of two or more, and another among 2,052 Americans aged 18 and older.
Data for the PCP survey were weighted where necessary by age, gender and specialty to bring them in line with their actual proportions in the population.
Data for the general population survey were weighted where necessary by age, gender, race/ethnicity, region, education, marital status, household size, household income and propensity to be online, to bring them in line with their actual proportions in the population.
Cost is a major concern
The findings published in the report “The Coming Alzheimer’s Disease Healthcare Revolution: US Physician and Adult Perspectives on the Future of Diagnostics and Treatment” suggest cost concerns could impede the adoption of blood tests for AD: more than 8 in 10 physicians (85%) say the value of a blood test for the early detection of AD risk will depend on how widely it is reimbursed.
However, 94% of physicians say blood tests would be more cost effective for the healthcare system compared to more invasive methods of detection (e.g., lumbar puncture, imaging studies).
“We are on the cusp of a new generation of therapies for Alzheimer’s disease, but the important role of diagnostics has been missing from the conversation.
“Patients today are typically screened for Alzheimer’s disease only after signs of cognitive impairment emerge and often by expensive methods, such as brain imaging and cerebrospinal fluid taps, which only specialists can perform,” said Michael K. Racke, MD, Neurology Medical Director, Quest Diagnostics.
“As new, efficacious therapies come to the forefront, the need for scalable, less invasive and more cost-effective diagnostics, including in primary care settings, will grow,” he said.
Could improve clinical trials
“Our goal for this report is to help prepare the medical community and engaged patients and caregivers for the transformational healthcare shifts that must occur to unleash the full potential of future treatment and diagnostic innovations to improve outcomes for patients with Alzheimer’s disease.”
According to the survey, 96% of physicians say blood tests will help identify patients who may be appropriate for clinical trials for AD treatments, and 85% say blood tests will improve the quality and speed of clinical trials.
The report follows a decision in April 2022 by the Centers for Medicare and Medicaid Services to limit coverage of the AD drug aducanumab to patients who receive it as participants in a clinical trial.
The Food and Drug Administration’s approval of the drug in June 2021 marked the first authorization of a treatment designed to target AD pathophysiology.
Can improve treatment
The identification of biomarkers for AD has led to new avenues of pharmaceutical drug research and development. More than 100 disease-modifying therapies are now in clinical trials – nearly 20 in phase 3.
The large majority of physicians (84%) say testing for early risk of AD will lead to earlier and improved disease management.
An even greater number of physicians (92%) say blood tests for AD will lead to a surge in diagnoses, however – with 60% saying the current healthcare system/workforce would not be able to handle a surge in diagnoses.
The vast majority of physicians (95%) noted that the value of a blood test depends on the quality of education around it.
SOURCE:
REFERENCE:
- 2021 Alzheimer’s Clinical Trials Report Accessed April 10, 2022.
- Li Y, Schindler SE, Bollinger, J, et al. Validation of plasma amyloid-β 42/40 for detecting alzheimer disease amyloid plaques. Neurology. Online ahead of print, December 14, 2021.doi:10.1212/WNL.0000000000013211