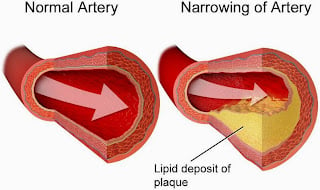
DALLAS – Vascular dementia commonly springs from strokes or similar cardiovascular events. A stroke can be triggered by too much “bad” cholesterol. It contributes to plaque, a thick, hard deposit that can clog arteries and make them less flexible. This condition is known as atherosclerosis. If a clot forms and blocks a narrowed artery, it can choke brain cells or cause a stroke. When enough brain cells are damaged this way, the result is vascular dementia.
Cholesterol Guidelines from AHA
A study from UT Southwestern researchers found that cholesterol guidelines, from the American College of Cardiology and the American Heart Association, would significantly reduce new cardiovascular events, when compared to treatment based on previous cholesterol guidelines.
The research identified Dallas Heart Study participants in the 30 to 65 age range who would have qualified for statin use under the cholesterol guidelines introduced in by the American College of Cardiology (ACC) and the American Heart Association (AHA).
In this subset of patients, the study predicted that 3.6 to 4.9 cardiovascular events would have been prevented for every 1,000 people screened and treated according to the new guidelines rather than the old guidelines (using a risk-reduction factor of 30 percent to 45 percent, depending on the statin dosage). The Dallas Heart Study is a multiethnic, population-based study of thousands of Dallas County adults whose cardiovascular health has been followed for 10 years.
Projecting these findings onto the larger Dallas County population, about 4,500 serious cardiac events would have been prevented in individuals 30 to 65 years of age over a 10-year period by following the new cholesterol guidelines.
When the new guidelines were introduced – replacing previous guidelines from the National Cholesterol Education Program/Third Adult Treatment Panel – they provoked heated debate over the sizeable increase in statin eligibility. However, the UT Southwestern study supports the merit of the new cholesterol guidelines, as well as increased statin use.
“This is one of the first studies to carefully predict the implications of the new guidelines in the general population beyond just the amount of increase in statin use,” said Dr. Amit Khera, Associate Professor of Internal Medicine and Director of the Preventive Cardiology Program at UT Southwestern. “Does it look like these new guidelines will prevent heart attacks and strokes? The answer is, ‘yes,’” he said.
Dr. Khera is senior author of the recently published study, which appeared inCirculation: Cardiovascular Quality and Outcomes.
The 2013 ACC/AHA Cholesterol Guidelines recommend statins for patients with existing atherosclerotic cardiovascular disease, type 2 diabetes, and very high levels of LDL cholesterol, as well as for patients with a high 10-year risk for heart disease.
The previous guidelines from the National Cholesterol Education Program/Third Adult Treatment Panel were based on a different formula that involved targeting specific cholesterol levels. Some patients fall out of statin eligibility under the new guidelines, but some 12.8 million more are newly eligible.
Among Dallas Heart Study participants who actually experienced a cardiovascular event, 37.1 percent more of those patients would have been placed on statins if the new guidelines had been in place. Among participants who did not experience a cardiovascular event, only 3.9 percent more patients would have been prescribed statins.
“There has been a lot of emphasis on the increased use of statins and a lot of emphasis on the risk calculator,” said Dr. Khera, who holds the Dallas Heart Ball Chair in Hypertension and Heart Disease. “Yes, there is some additional statin use, but according to our results, this use seems appropriate, at least in this age group.”
The Dallas Heart Study was funded by the Donald W. Reynolds Foundation and is partially supported by the National Center for Advancing Translational Sciences of the National Institutes of Health.
Other UT Southwestern researchers involved in this study are first author Dr. Andre Paixao, a former UT Southwestern Cardiology Fellow and current Interventional Cardiology Fellow at Emory University; Colby Ayers, Faculty Associate in the Department of Clinical Science; Dr. Jarett Berry, Assistant Professor of Internal Medicine and Clinical Science; and Dr. James de Lemos, Professor of Internal Medicine, Associate Program Director of the Cardiology Fellowship Program, and holder of the Sweetheart Ball – Kern Wildenthal, M.D., Ph.D., Distinguished Chair in Cardiology.
SOURCE:
UT Southwestern Medical Center
UT Southwestern, one of the premier academic medical centers in the nation, integrates pioneering biomedical research with exceptional clinical care and education. The institution’s faculty includes many distinguished members, including six who have been awarded Nobel Prizes since 1985. Numbering more than 2,700, the faculty is responsible for groundbreaking medical advances and is committed to translating science-driven research quickly to new clinical treatments. UT Southwestern physicians provide medical care in 40 specialties to nearly 91,000 hospitalized patients and oversee more than 2 million outpatient visits a year.