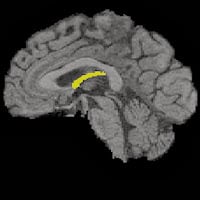
The fornix is a small, wishbone-shaped structure deep inside the brain. It provides a person’s earliest clues to future cognitive decline. Find out how much it can reveal long before memory loss or dementia appear.
A key study by researchers with the UC Davis Alzheimer’s Disease Center has found that the degeneration of a small, wishbone-shaped structure deep inside the brain may provide the earliest clues to future cognitive decline.
The longitudinal study found that the only discernible brain differences between normal people who later developed cognitive impairment and those who did not were changes in their fornix, an organ that carries messages to and from the hippocampus, and that has long been known to play a role in memory.

A brain showing the fornix structure highlighted.
“This could be a very early and useful marker for future incipient decline,” said Evan Fletcher, the study’s lead author and a project scientist with the UC Davis Alzheimer’s Disease Center.
“Our results suggest that fornix variables are measurable brain factors that precede the earliest clinically relevant deterioration of cognitive function among cognitively normal elderly individuals,” Fletcher said.
The research is published online in JAMA Neurology.
Hippocampal atrophy occurs in the later stages of cognitive decline and is one of the most studied changes associated with the Alzheimer’s disease process. However, changes to the fornix and other regions of the brain structurally connected to the hippocampus have not been as closely examined. The study found that degeneration of the fornix in relation to cognition was detectable even earlier than changes in the hippocampus.
“Although hippocampal measures have been studied much more deeply in relation to cognitive decline, our direct comparison between fornix and hippocampus measures suggests that fornix properties have a superior ability to identify incipient cognitive decline among healthy individuals,” Fletcher said.
The study was conducted over five years in a group of 102 diverse, cognitively normal people with an average age of 73 who were recruited through community outreach at the Alzheimer’s Disease Center. The researchers conducted magnetic resonance imaging (MRI) studies of the participants’ brains that described their volumes and integrity. A different type of MRI was used to determine the integrity of the myelin, the fatty coating that sheaths and protects the axons. The axons are analogous to the copper wiring of the brain’s circuitry and the myelin is like the wiring’s plastic insulation.
Either one of those things being lost will “degrade the signal transmission” in the brain, Fletcher said.
The researchers also conducted psychological tests and cognitive evaluations of the study participants to gauge their level of cognitive functioning. The participants returned for updated MRIs and cognitive testing at approximately one-year intervals. At the outset, none of the study participants exhibited symptoms of cognitive decline. Over time about 20 percent began to show symptoms that led to diagnoses with either mild cognitive impairment (MCI) and, in a minority of cases, Alzheimer’s disease.
“We found that if you looked at various brain factors there was one — and only one — that seemed to be predictive of whether a person would have cognitive decline, and that was the degradation of the fornix,” Fletcher said.
The study measured two relevant fornix characteristics predicting future cognitive impairment — low fornix white matter volume and reduced axonal integrity. Each of these was stronger than any other brain factor in models predicting cognitive loss, Fletcher said.
He said that routine MRI examination of the fornix could conceivably be used clinically in the future as a predictor of abnormal cognitive decline.
“Our findings suggest that if your fornix volume or integrity is within a certain range you’re at an increased risk of cognitive impairment down the road. But developing the use of the fornix as a predictor in a clinical setting will take some time, in the same way that it took time for evaluation of cholesterol levels to be used to predict future heart disease,” he said.
Fletcher also said that the finding may mark a paradigm shift toward evaluation of the brain’s white matter, rather than its gray matter, as among the very earliest indicators of developing cognitive loss. There is currently a strong research focus on understanding brain processes that lead eventually to Alzheimer’s disease. He said the current finding could fill in one piece of the picture and motivate new directions in research to understand why and how fornix and other white matter change is such an important harbinger of cognitive impairment.
“The key importance of this finding is that it suggests that white matter tract measures may prove to be promising candidate biomarkers for predicting incipient cognitive decline among cognitively normal individuals in a clinical setting, possibly more so than gray matter measures,” he said.
Other study authors are Mekala Raman, Philip Huebner, Dan Mungas, Owen Carmichael and Charles DeCarli of UC Davis and Amy Liu of UC Davis and the Novartis Institutes for BioMedical Research.
The study was funded by grants from the National Institute on Aging (P30 AG10129; U01 AG024904; R01 AG010220 and 2R01 AG021028).










There are hundreds of research articles that shows ths neuroproctetive effects of small doses of ACETYL-L-CARNITINE (so called ALCAR), in neurons cells cultures, in animal models research, and in human being trials of patients with Alzheimer disease and others dementias , proved by research made in the lasts forty years.
The Fimbria-fornix Transection in adult rats results in degeneration of the Hippocampal cholinergic pathway, reminiscent of that occurring in aging as well as Alzheimer disease.
In the reference research articles bellow, can see that ACETYL-L-CARNITINE, RESTORED FORNIX FUNCTION , and Acetylcholine and Nerve Growth Factor Activity in the HIPPOCAMPUS of rats with Partial (1) or Total (2) Transection of the FIMBRIA-FORNIX bundle.
1) International Journal of Developmental Neuroscience in 1995 February, with the title "Acetyl-L-Carnitine Restores Choline Acetyltransferase Activity in the Hippocampus of Rats with PARTIAL UNILATERAL FIMBRIA-FORNIX TRANSECTION", authors Piovesan and colleagues.
2) Journal of Brain Research, 1994 January, title: "Acetyl-L-Carnitine Treatment Increases Choline Acetyltransferase Activity and Nerve Growth Factor levels in the Central Nervous System of adult rats following TOTAL FIMBRIA-FORNIX TRANSECTION." Authors Angelucci L and colleagues.
The very very low doses of acetyl L carnitine, (unlike the sites that sells acetyl Lcarnitine supplements uses to reccomends) , the safest and best doses are the lowest doses, with capsules with doses between eighty miligrams to one hundred miligrams, three times a day, after main mewls, up to, 5:00 P. M., but that are empirical doses.
To use any nutraceutical supplement it is only under PHYSICIAN permission and supervision .
Only yhe physician of the patient can gives permision to use acetyl L carnitine and knows the best doses for each patient.